by Saniya Lee Ghanoui | Jun 17, 2014 | Birth Control, Communication, Health Care
Guest Post by Jennifer Aldoretta There seems to be a growing disconnect in recent years between physicians and their patients, and women are especially susceptible to this given our reliance on doctors for information about contraception. When compared to the...
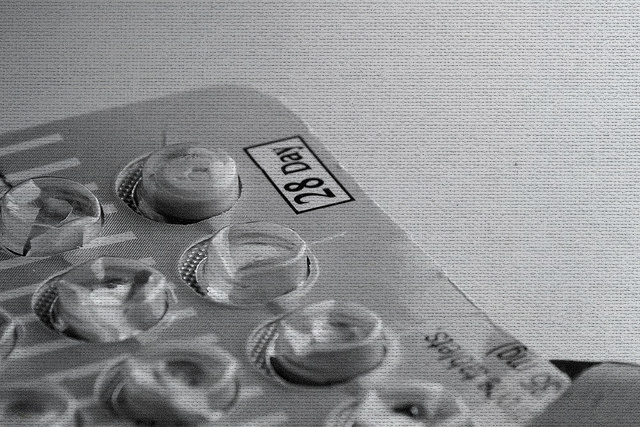
by Kati Bicknell | Jan 15, 2013 | Birth Control, Fertility, Menstruation
Here’s a notion: Birth control pills are not the only way manage your reproductive health. The pill came out more than 50 years ago, and at the time, it was a symbol of liberation and freedom for women. Suddenly, they no longer had to worry about unplanned pregnancy....
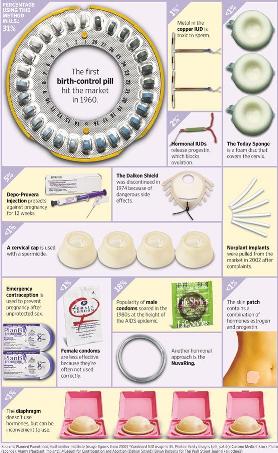
by Laura Wershler | Apr 20, 2010 | Birth Control, Newspapers, Pharmaceutical, Philosophy
I read The Birth-Control Riddle by Melinda Beck, published today in The Wall Street Journal with interest and frustration. As a veteran pro-choice sexual and reproductive health advocate, I’ve spent decades contemplating this “riddle”. I have two specific...
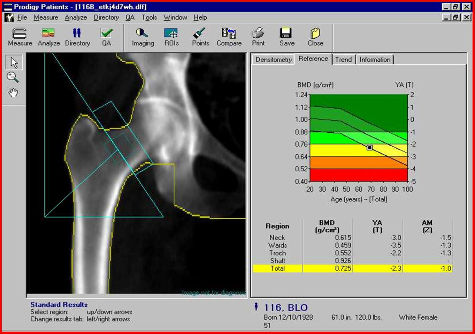
by Elizabeth Kissling | Dec 27, 2009 | Birth Control, New Research, Pharmaceutical
New research from the University of Texas Medical Branch at Galveston finds that nearly half of women using depot medroxyprogesterone acetate (DMPA), commonly known as the birth control shot, will experience high bone mineral density (BMD) loss in the hip or lower...
by Elizabeth Kissling | Sep 26, 2009 | Law/Legal, Newspapers, Pharmaceutical
The popular birth control pill, Yaz is in the news again. Readers may remember that last autumn, Bayer (the maker of Yaz) was sanctioned by the FDA for their television commercials, “because they encourage use of Yaz in circumstances other than those in which...



