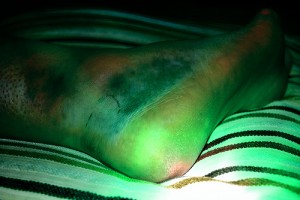
About two weeks ago, I injured my foot. Like many accidents, it was stupid, quick, and avoidable. A heavy storm door was swinging shut, I somehow didn’t get out of its way, and it sheared open the back of my left foot, behind the ankle. Luckily, I didn’t cut an artery, the Achilles tendon, or any other tissue that would have caused a crisis or long-term problem. However, I did end up with eleven stitches and orders to stay off my feet for over a week.
If life gives you lemons, make lemonade. During my enforced inactivity, I surrounded myself with projects I had not had time for. The reverse appliqué hand sewing I had started in a class last summer but never finished. A creative writing project I had hoped to do. My long-neglected Native American flute. Yet, as the days wore on, I found myself increasingly unable to do much more than stare into space, watch TV, or do a bit of sewing. It was hard to focus my attention and to concentrate; I felt an increasing paralysis of will to initiate and sustain activity. When I did walk around, using crutches to keep weight off my foot and to avoid flexing the ankle, I felt easily fatigued and vaguely ill.
I did also do some reading, and happened upon a recent re-evaluation of a book by Oliver Sacks called “Leg to Stand On”. Sacks, a neurologist, had written the book in 1984 after he broke his leg in a traumatic accident. He found, to his surprise, that his injury resulted in important changes in his body image. In the early part of his recovery, his leg did not feel like part of him. Although he couldn’t feel or voluntarily move the leg, and couldn’t even remember moving it in the past, it could move in response to music. He later discovered that his experience was shared by other patients. In the re-evaluation, authors Stone, Perthen, and Carson suggest that Sacks’ problem was functional (i.e., psychological not physical). Sacks, in response to their reevaluation, suggests that activity and sensation in the periphery—that is, arms and legs—is intrinsically involved in how the central nervous system organizes information, experience, and cognitive function. That is, the mind and entire body are interconnected.
There are many ways in which physical experiences other than injuries have broad systemic, mind/body interconnections. If we have a fever, we’re not surprised if, in addition to our stomachs hurting or our heads throbbing, we feel wonky, unable to concentrate, distressed. Illness is a whole-body experience. Many years ago, I had an amniocentesis. The doctor told me I could go about my business after he finished the procedure, but a nurse said to me that many people felt they needed some rest. Indeed, after having a large needle penetrating my abdomen, which felt, irrationally but unmistakably, like an invasion of body boundary, I did feel shaken and like I needed to recupe. Even my husband, a physicist, a very nice but definitely not a touchy-feely kind of guy, felt invaded by a large needle penetrating his body to take a bone marrow sample.
So it is with uncomfortable experiences associated with the menstrual cycle. Menstrual cramps, hot flashes, and menstrual migraines are not isolated symptoms occurring in far-out or isolated body parts. If we have menstrual cramps, we may be tensing our entire body, our abdomens may feel like invaded strangers rather than like parts of ourselves, the cramps may have specific meanings about who we are, our lives, or the meaning of pain or discomfort. If I have menstrual migraines, I may wonder why people don’t show me more sympathy and help me, or I may want to keep my headaches secret. Not always, but often, menstrual cycle experiences, like many other experiences, are holistic, mind/body phenomena.
References
Sacks, O. (2012). The Central Effects of Peripheral Injury. Journal of Neurol. Neurosurg. Psychiatry, vol. 83, p. 868. Downloaded from www.medscape.com/viewarticle/769178.
Sacks O. (1984). A Leg to Stand on. New York: Harper & Row, 1984.
Stone, J., Perthen, J., & Carson, A. (2012). ‘A Leg to Stand On’ by Oliver Sacks: A reappraisal: The diagnosis reappraised—functional paralysis? Journal of Neurol. Neurosurg. Psychiatry, vol. 83, pages 864-867. Downloaded from www.medscape.com/viewarticle/769177.