Guest Post by Jerilynn Prior, M.D. — Centre for Menstrual Cycle and Ovulation Research
By “midlife muddle” I don’t mean the trouble concentrating or remembering names that sometimes occurs for all of us (but more frequently if we’ve wakened with night sweats and not gotten back to sleep). I mean the condoned and official confusion about naming of women’s reproductive aging. Let me show you why I am upset.
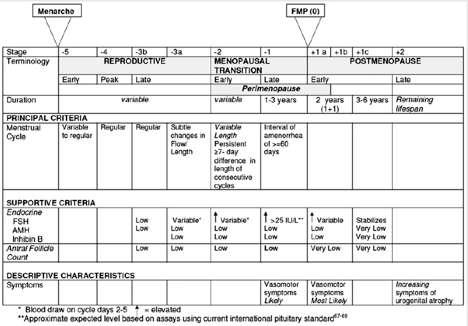
Stages of Reproductive Aging Workshop (STRAW) held a 10-year anniversary last summer. (As someone frustrated by not being “heard” at the original conference, I still think that the “W” in STRAW should stand for Women!) Despite that, STRAW+10 has made progress because at least some of the classification is now supported by population-based prospective data rather than based on what experts believe. The names that are now politically correct are summarized in the STRAW+10 Executive Summary1 and the diagram1 at right.
We in the Society for Menstrual Cycle Research have also had our say about nomenclature: “Naming Women’s Midlife Reproductive Transition”. I wrote this (with revision and refinement by collective effort of SMCR members) because women keep getting left out of this naming business. For example:
- a regularly menstruating woman with night sweats, heavy flow, and increased cramps could learn to call herself perimenopausal2 (not STRAW+10 Late Reproductive Phase -3b?!).
- a woman who just finished her period can say, I’m in late perimenopause and have at least a year without further flow before I’ll be menopausal. Based on STRAW+10 she could be told that specific menstruation was her final menstrual period (nickname “FMP”) and the next day, according to STRAW+10 be told that she is now “postmenopausal”!!
- a woman with sore breasts, irregular periods, and heavy flow could say, I’m in perimenopause. However, she may instead be told she is in the “Early Menopausal Transition.” Because she has heavy flow she is also likely to be prescribed the birth control pill (as is currently and commonly recommended). Usually she will not be told that The Pill will make her perimenopausal irregular flow worse—she may well start spotting in the middle of her cycle.3
This new and improved STRAW+10 still centers all of women’s reproduction on that mythical FMP. But to call the FMP “menopause”, as many women’s health experts do, is just unscientific. It takes at least a year without another menstruation in those of us over age 45 before nine out of ten of us will not get another period4. But one (out of ten) of us will get a further, normal period even though we’ve been that whole year without any4. We can tell that new flow is normal (in other words, does not need investigation for endometrial cancer) if we had cramps or bloating or sore breasts or moodiness—or all of these—that told us our period was coming.
So our new Naming position statement says don’t call it “menopause” until you’ve not had a period for a year. And do call it “perimenopause” if things are variable and changing even if you are still having regular flow2. Three of nine changes can confirm for you that you are perimenopausal even if your flow is still regular:2
- Shorter cycles (25 days or less);
- Increased cramps;
- Heavier flow;
- Increased trouble sleeping—especially waking up in the middle of sleep;
- New or increased migraine headaches;
- Night sweats—especially if they tend to occur before or during flow;
- An increase in or new premenstrual mood swings;
- New sore, enlarging or nodular breasts; and
- Weight gain without changes in what you eat or the exercise you do.
If women can learn to call themselves perimenopausal, they will be saying they know that perimenopause is not the same as menopause—perimenopause is a midlife transition with higher and erratic estrogen levels. Menopause is a fairly stable life phase with normally low estrogen and progesterone levels that begins one year after their last menstrual flow.
Furthermore, by naming themselves accurately they will be able to tell whether a medication that is proposed for them has been tested and proven effective in perimenopausal women. Usually symptomatic women are treated with oral contraceptives (that are proven reasonably safe and useful for premenopausal contraception), or offered hormone therapy that has only been tested and shown effective for hot flushes/flashes in menopausal women.
So. . . I like the word, perimenopause and think if women understand and own it they will be on their way out of a midlife muddle.
References
- Harlow, S. Executive Summary of the Stages of Reproductive Aging Workshop +10: addressing the unfinished agenda of staging reproductive aging [pdf]. Fertility Sterility, 2012 doi: 10.1016/j.fertnstert.20012.01.128
- Prior JC. Clearing confusion about perimenopause. BC Med J 2005; 47(10):534-538.
- Casper RF, Dodin S, Reid RL, Study Investigators. The effect of 20 ug ethinyl estradiol/1 mg norethindrone acetate (MinestrinTM), a low-dose oral contraceptive, on vaginal bleeding patterns, hot flashes, and quality of life in symptomatic perimenopausal women. Menopause 1997; 4:139-147.
- Wallace RB, Sherman BM, Bean JA, Treloar AE, Schlabaugh L. Probability of menopause with increasing duration of amenorrhea in middle-aged women. Am J Obstet Gynecol 1979; 135(8):1021-1024.


Mirena is not yet a standard recommendation for heavy flow? I love mine.
I wonder if this confusion about perimenopause vs menopause has to do with the different ways hormone therapy is prescribed? It sort of makes sense since women who have their ovaries removed get worse symptoms than women with with natural menopause. In this case, these women aren’t really going through the “puberty-in-reverse” transition; they just fall off a cliff and get horrible estrogen withdrawal. So it seems our thinking has been cemented this way for so long because the women with natural menopause, whose symptoms tend to be less severe, are seen as going through slower estrogen withdrawal (perimenopause). In this sense, the true hormonal chaos of perimenopause is doomed for misunderstanding because people think it’s DROPPING estrogen levels that cause the misery.
What might be even more important in this argument is the TYPE of women who require hysterectomy/oophorectomy. These women are undoubtedly on estrogen overload, either because of their weight or something else. But nevertheless, the heavy bleeding/endometriosis/whatever that precipitates the need for the surgery never gets addressed. Why? Because as soon as they have the surgery, they get prescribed yet MORE unopposed estrogen (usually Premarin). As for women with natural menopause (and therefore a perimenopause), they too end up falling prey to the estrogen-deficieccy medical model since their transition is seen as the less-severe equivalent to oophorectomy.
Sadly, progesterone ends up being a minor player in this picture. For women with natural menopause, it’s seen as the tagalong for uterine protection, but otherwise, it’s estrogen that’s supposedly the miracle cure-all. As for women with surgical menopause, progesterone is seen as having absolutely NO ROLE in their symptom management. Since they no longer have a uterus, so the thinking goes, they just need estrogen. ? If the recent trial evidence showing that progesterone helps sleep, hot flashes, and night sweats in menopausal women is any indication, might it be progesterone that keeps younger, premenopausal women from having hot flashes in the first place despite the major estrogen increases and decreases thoughout their cycles? And might it be progesterone as a therapy that could help women avoid hysterectomy who would have otherwise need it in the first place? If these questions were thoroughly explored, as Dr. Prior has spent her career doing, I think HER defintions of perimenopause/menopause would rightfully be in textbooks.
Hi Pamsc,
I’m glad that the levo-norgestrel impregnanted IUD is working for you–it is very good at helping heavy flow.
The only disadvantage for a perimenopausal woman trying to understand what’s going on for herself is that the LNG-IUD may take away flow and thus obscure the true end of perimenopause and the beginning of menopause.
Another disadvantage of LNG-IUD, for women who have sleep problems or night sweats, is that it doesn’t address these at all.
Thanks,
Thanks, JR.
I think you are perceiving something that is very important and not discussed. The differences between the perimenopausal women who end up having hysterectomies and those that don’t are not only the higher estrogen/lower progesterone levels causing their heavy flow, endometriosis, fibroid-growth but also the knowledge about what is happening for them.
You should know that, after years of using progesterone as a treatment for symptomatic perimenopausal women to counteract the tissue effects of high estrogen (which is progesterone’s “job” as I see it!), I finally have achieved two things:
1) A peer reviewed paper that discusses why and how to use progesterone therapy for symptomatic perimenopause–you can access the whole article through the following link: https://www.cemcor.ubc.ca/files/uploads/Prior_2011_Progesterone_Symptomatic_Perimeno.pdf
2) We are doing a randomized double-blind placebo controlled trial of oral micronized progesterone for hot flushes and night sweats in perimenopausal women.
Thanks for your thoughtful comments, JR
Jerilynn–With regard to the idea that “STRAW+10 has made progress because at least some of the classification is now supported by population-based prospective data rather than based on what experts believe”– There is some population-based data, but the STRAW+10 article did not address complexities found in the research that the ReStage group, which tested STRAW classifications, came up with (e.g., The ReStage Collaboration: defining optimal bleeding criteria for onset of the early menopausal transition,” Harlow et al., “Menopause,” vol. 89, 2008). For example, the 7-day criterion for entry into early transition did not predict the final menstrual period for women under 40 (although the median age for meeting the criterion was age 41 so many women must have met it before age 40, and the rationale for the 7-day criterion was it corresponds to physiological changes found in the late thirties). Also, the age groups for early and late transition overlapped in ways the authors found problematic in terms of these being separate, invariant stages.
Yes, Paula,
I hadn’t recalled the age issue in the ReStage paper.
The idea of making set criteria for perimenopause based on menstrual cycle criteria is very problematic. Women’s reproductive transition is not a set of stairs that we climb. That’s why I like to call them “phases” which sounds more biological and organic. They are most like seasons–it can start to feel like spring and then snow!
Years and years ago Patricia Kaufert (U. of Manitoba) discovered in tracking cycles prospectively that there were over 100 different patterns in about 300 women! A woman may reach criteria for late menopause transition and then revert to an regular menstrual cycle for many months! Or may have 12 months of no flow and get another period (as 10% of women over 45 do and at least 20% of women 45 and younger do).
Data from the Tremin Trust started by Treloar (reported by Phyllis Mansfield–Mansfield PK, Carey M, Anderson A, Barsom SH, Koch PB. Staging the menopausal transition: data from the TREMIN Research Program on Women’s Health. Womens Health Issues 2004; 14(6):220-226) showed the same thing–you get to a certain point and then may move back to earlier cycle pattern.
Thanks for reminding us of what the data show.
Jerilynn