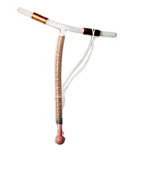
 In our pill popping economy, the go-to option for long term birth control has, since the late 1970’s, been the pill. In the 1970’s the copper IUD (Intrauterine Device) fell out of favor after recalls, cases of infection and cases of sterilization. However, this recent Newsweek article, The IUD Reborn by Meredith Melnick suggests that the IUD is on the rise. The article cites both ParaGard (the copper IUC) and Mirena (the hormonal IUD by Bayer) as making comebacks, building from a Virginia Commonwealth study that “surveyed women with clinically defined “high-risk” sexual behavior (one third had documented histories of sexually transmitted disease), and found that modern IUDs do not increase the rate of pelvic inflammatory disease or infertility among women who have multiple partners or contract STDs. Some of the study’s data suggested that the Mirena actually protects against STDs by causing an overproduction of cervical mucus, which can act as a barrier to pathogens.”
In our pill popping economy, the go-to option for long term birth control has, since the late 1970’s, been the pill. In the 1970’s the copper IUD (Intrauterine Device) fell out of favor after recalls, cases of infection and cases of sterilization. However, this recent Newsweek article, The IUD Reborn by Meredith Melnick suggests that the IUD is on the rise. The article cites both ParaGard (the copper IUC) and Mirena (the hormonal IUD by Bayer) as making comebacks, building from a Virginia Commonwealth study that “surveyed women with clinically defined “high-risk” sexual behavior (one third had documented histories of sexually transmitted disease), and found that modern IUDs do not increase the rate of pelvic inflammatory disease or infertility among women who have multiple partners or contract STDs. Some of the study’s data suggested that the Mirena actually protects against STDs by causing an overproduction of cervical mucus, which can act as a barrier to pathogens.”
I hope this copper IUD resurgence proves true, for the device has been so tainted that obtaining one sometimes proves quite a feat of strength on the part of the client. Not only might one have to ask for a non-hormonal IUD by name (“I’ll take ParaGard, please. No, the copper one.”) you may need to explain why you are choosing this device (“Birth control at a fraction of the cost, normal ovulation, 99.2%-99.9% effective, etc.”) In my experience, and in the cases of other recent IUD recipients, we needed to coach our gynecologists through the process of insertion. A friend who obtained an IUD this week reported to me that, while in stirrups waiting for the procedure to begin, she noticed her gynecologist reading the instructions on the package. She asked him if he knew what he was doing and he said, with some degree of uncertainty, “Oh yes. They’ve just changed the packaging.” My own gynecologist admitted that she needed to re-read the packaging as well for she inserts less than one IUD per month at her hopping New York City clinic.
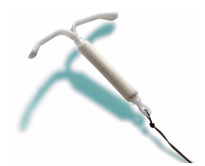 Finally, to get coverage from an insurance company, in some cases you must convince them to cover the device (of course, this is if you are lucky enough to have insurance.) Conversations may go something like this: “No. I cannot buy a copper IUD at the drug store and bring it to my gynecologist. I must order it directly from the company and they ship to the gynecologist. And yes, you WILL reimburse me for this charge.” Then, they may not reimburse you, and in that case I recommend putting up a fight. Mine included writing a letter laying out the costs of other birth control options. “My gynecologist prescribed this device to me as a safe, non-hormonal contraceptive that is effective for 10 years. I will not need hormonal pills for those 10 years and will not incur additional expenses based on failure of a hormonal product. If you calculate the savings you accrue, based on my choice to use a non-hormonal IUD, it is quite significant.” Needless to say, I received the check in the mail two weeks later without apology.
Finally, to get coverage from an insurance company, in some cases you must convince them to cover the device (of course, this is if you are lucky enough to have insurance.) Conversations may go something like this: “No. I cannot buy a copper IUD at the drug store and bring it to my gynecologist. I must order it directly from the company and they ship to the gynecologist. And yes, you WILL reimburse me for this charge.” Then, they may not reimburse you, and in that case I recommend putting up a fight. Mine included writing a letter laying out the costs of other birth control options. “My gynecologist prescribed this device to me as a safe, non-hormonal contraceptive that is effective for 10 years. I will not need hormonal pills for those 10 years and will not incur additional expenses based on failure of a hormonal product. If you calculate the savings you accrue, based on my choice to use a non-hormonal IUD, it is quite significant.” Needless to say, I received the check in the mail two weeks later without apology.
Thankfully, while IUD questions and problems arise, there are helpful discussion boards like IUD Divas. As with hormonal birth control pills, you are still at risk for contracting STD’s. Condoms, dental dams, gloves and the like must still be part of any non-monogamous sexual practice. But this is an interesting development and it will be followed here. For, as with the diaphragm, inexpensive birth control options seem to fall far out of favor when there are expensive pills to be swallowed en masse.


I got a Paragard IUD two years ago and I fucking LOVE IT. Hassle free, I got to go off the damn pill, and I’m saving tons of money. I named it Washington. :3 Since then, my sister and BFF have also gotten IUDs (one Mirena, the other Paragard) and they love them too!
I’ve been off the pill for a few years after deciding I didn’t like weird chemical messing with my ovulation. I have not been having sex regularly, so I have been relying on condoms, and on one occasion the day after pill (as hormones are still better than being pregnant in my opinion)
I’ve been looking into getting a copper IUD. I’m lucky enough to be in a big city with a planned parenthood. I’m going there instead of my GP or OBGYN because I figure they deal with birth control every day, and are likely to have more accurate information and more practice.
While I can appreciate that this was true for you and is likely true for others as well, it’s not really a universal experience (as phrasing it with only a general “you” might make it seem). When I asked my NP for an IUD, the conversation went something like this:
Me: I’d like to get an IUD.
NP: Which one?
Me: ParaGard, the copper one.
NP: Sure. I’d like to take swabs for gonorrhea and chlamydia to make sure there are no bacterial STIs at the time of insertion. Here is some literature on IUDs, including benefits and risks. Look through it, feel free to ask questions, and we’ll call to schedule an insertion appointment as soon as the test results come back from the lab.
I had the Flexi-T IUD inserted recently and so far it’s going great. Though I think the copper IUD making a comeback after years of low use might only be true for North America. I recently read an article about it being very popular in some countries, China being one specifically named as having very high rates of use.
@Tori. Thanks for your comment. I wish I had your physician! Have changed the post to reflect your feedback.
I cannot use hormonal, don’t trust barrier, and was bullied for using FAM, so I opted for a IUD as a way to avoid harassment from GP’s. My first GP had refused me a IUD as he claimed it’d leave me infertile, and I wasn’t happy about the idea of having something so unnatural inside my uterus, I even had a small issue of both my IUD’s being expelled (either my bodies reaction or my using the wrong menstrual cup). But after years using a IUD I can say I actually like it.
What surprised me, after so many years of GP’s trying to force me onto the pill, I found many gyno’s and nurses in GUM/family planning clinics seemed to absolutely LOVE the idea of IUD’s and wanted more women to start using them. I have noticed the NHS is pushing the idea of IUD’s more these days too.
IUD use is definitely on the rise in Canada. The sexual health clinic where I live is now offering a half day clinic each week dedicated to IUD insertions and follow-up. They are doing both copper and Mirena. One other interesting note: anecdotal evidence suggests that many women are choosing IUDs post-abortion. More than a few because they got pregnant while using hormonal contraception, even though they assert they were using it correctly. It well could be that the typical use effectiveness rate of the pill(patch?, ring?)is dropping significantly. The IUD resurgence is also evidence of a push-back against hormonal contraception. Let’s face it, if the pill was so great, everyone would be taking it without complaint or concern.