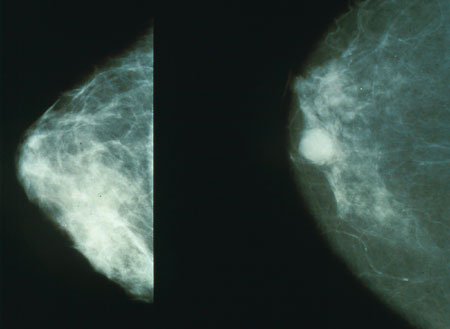
Mammograms showing healthy (left) and (right) cancerous breast. Courtesy of the National Cancer Institute.
Can having too many menstrual cycles give you breast cancer? That’s what one might conclude from two unrelated articles that appeared in national newspapers this week.
First was Nicholas D. Kristof’s Op-Ed in the New York Times. Kristof had recently attended a symposium exploring whether certain common chemicals are linked to breast cancer and other ailments. The role of estrogen – both the real thing our bodies produce and the pseudo-estrogens – in breast cancer was his major example.
The real thing:
One theory starts with the well-known fact that women with more lifetime menstrual cycles are at greater risk for breast cancer, because they’re exposed to more estrogen. For example, a woman who began menstruating before 12 has a 30 percent greater risk of breast cancer than one who began at 15 or later.
The pseudo-estrogens:
One class of chemicals that creates concern — although the evidence is not definitive — is endocrine disruptors, which are often similar to estrogen and may fool the body into setting off hormonal changes. This used to be a fringe theory, but it is now being treated with great seriousness by the Endocrine Society the professional association of hormone specialists in the United States. …These endocrine disruptors are found in everything from certain plastics to various cosmetics.
(Do you ever wonder, like I do, why the birth control pill is not considered an ‘endocrine disruptor’ when that is exactly what it is?)
The second mention of the connection between too many periods and breast cancer came in dietician Leslie Beck’s Food For Thought column in Canada’s Globe and Mail. She was reporting on a new study showing that women with breast cancer need not shun soy:
By acting like weak forms of the body’s own estrogen, some experts have worried that soy isoflavones could possibly promote cancer growth. That’s because certain risk factors for breast cancer, such as beginning your menstrual period before age 12 or starting menopause after 55, are related to the length of time breast cells are exposed to the body’s own circulating estrogen. It’s thought that estrogen can promote the growth of breast cancer cells.
It’s reasonable to think that the both the writers and readers of these articles (and the many more that have surely mentioned this connection) might assume from this information that too many menstrual cycles means too much estrogen, therefore too many menstrual cycles must be a bad thing. What they don’t know is that not all menstrual cycles are created equal. It’s not necessarily about quantity, it’s about quality.
Common belief is that all menstrual cycles are ovulatory. (Unless, of course, you are using a hormonal birth control method that suppress ovulation like the pill, patch or ring.) In other words, the assumption is that if get your period you must have ovulated. This assumption is challenged by UBC endocrinolgist Jerilynn Prior, MD, and Scientific Director of the Centre for Menstual Cycle and Ovulation Research (CeMCOR). In her article Is Ovulation (and are normal Progesterone levels) Important for the Health of Women?, Dr. Prior has this to say about the connection between ovulation, menstruation and breast cancer:
What about history of ovulation problems and breast cancer? On this question, we have few good answers. Remember that we said it is commonly and wrongly understood that regular cycles mean normal ovulation? We know that women with more years of menstrual cycles (earlier first period, later menopause) have a higher risk for breast cancer (10).But we also know that regular cycles can be anovulatory and without progesterone. Compared with controls who had other reasons for infertility all of whom were followed through 1978, women with ovulation disturbances showed 5.4 times increased risk for premenopausal breast cancer. The second study observed all 1270 women hospitalized for AAE/PCOS at the Mayo Clinic beginning in the 1930s and compared their risk until the late 1970s with women hospitalized for other reasons. The women with chronic anovulation and androgen excess (AAE/PCOS) had a risk for menopausal breast cancer that was 3.6 times higher than their controls. Both of these studies suggest that chronic ovulation disturbance (especially if estrogen levels are normal or high as they are in AAE/PCOS) is an important risk for breast cancer.
Here is what’s critical about understanding the difference between ovulatory and anovualtory (no ovulation) menstrual cycles. Simply put, in ovulatory cycles estrogen is balanced by progesterone; in anovulatory cycles estrogen is not balanced by progesterone. Why is this important? Because the basic endocrinology of the menstrual cycle tells us that the rise of estrogen, prior to ovulation, stimulates the proliferation of breast cells (as well as every tissue in the body) and the progesterone during the second half of the cycle transforms and reduces that overgrowth.
The problem of too much estrogen therefore, is not one of too much ovulation or too many cycles, but rather one of too many ovulatory disturbances. And the reasons for ovulatory disturbances are many and varied: decreased emotional, economic or environmental security, excess/inadequate nutrition or illness, stress, diet, and as Kristof noted, exposure to environmental toxins and chemicals with estrogen-like properties. Beck, the dietician, might not realize that her sound nutritional advice, if followed, helps women achieve important health benefits in part because good nutrition fosters more consistent ovulatory menstrual cycles.
In her new book, The Estrogen Errors: Why Progesterone is Better for Women’s Health, (co-written with Susan Baxter, PhD) Dr. Prior devotes the last chapter to “Breasts, Breast Cancer, and Overcoming Our Fears”. She postulates that counterbalancing estrogen with sufficient progesterone could protect against breast cancer. The research presented in support is compelling. It is worth noting that Dr. Prior has developed a clincial protocol for cyclic progesterone therapy to counteract the effects and treat the many symptoms of high estrogen levels.
I expect we will continue to see, in articles and columns for some time to come, this free-floating assertion “that women with more lifetime menstrual cycles are at greater risk for breast cancer.” But if you’ve made it through this post, you won’t be the reader who worries that you started your period too young or wishes for menopause to come early. However, what you may want to do is learn how to determine if you are ovulating consistently yourself.


AHJ is interested in partners in the medicine genre. AHJ is a medicine web site which contains three thousand of high quality health care videos. We are looking for blog owners who may be interested in contributing guest blogs to our site. Please get in touch with us at our contact form on our web site.